
A digital world reveals new possibilities for medicine
Just over a decade ago, Fitbit made fitness-tracking fashionable—and the concept of digital health exploded on the consumer scene.
Today, while the digital health industry continues to engage consumers at extraordinary levels, it’s also spawning sophisticated devices that provide scientists and doctors with rich, personalized health information that’s never before been available.
With the help of body sensors, activity trackers and digital imaging tools, patients are partnering with the research world to shape a new era of data-driven discovery.
“Science, technology and medicine are now intersecting in ways that allow us to understand and take ownership of our own health information, and make new connections about factors that underlie health and disease,” says Eric Topol, MD, founder and director of Scripps Research Translational Institute and executive vice president of Scripps Research.
Digital health technologies are also enhancing early disease detection and “democratizing” medicine for those with limited access to nearby care. Topol, who is also a practicing cardiologist, and his team are combining the latest wearable devices with genomic technologies and advances in artificial intelligence to transform the future of medicine and human wellness.
“Information is power, and we’re only at the beginning of what’s possible,” Topol says. “There’s never been more promise or opportunity to reboot the way healthcare is managed.”
Science in a digital world
The growing ability to collect data from patients in real time is powerfully shaping the next phase of personalized medical treatments.
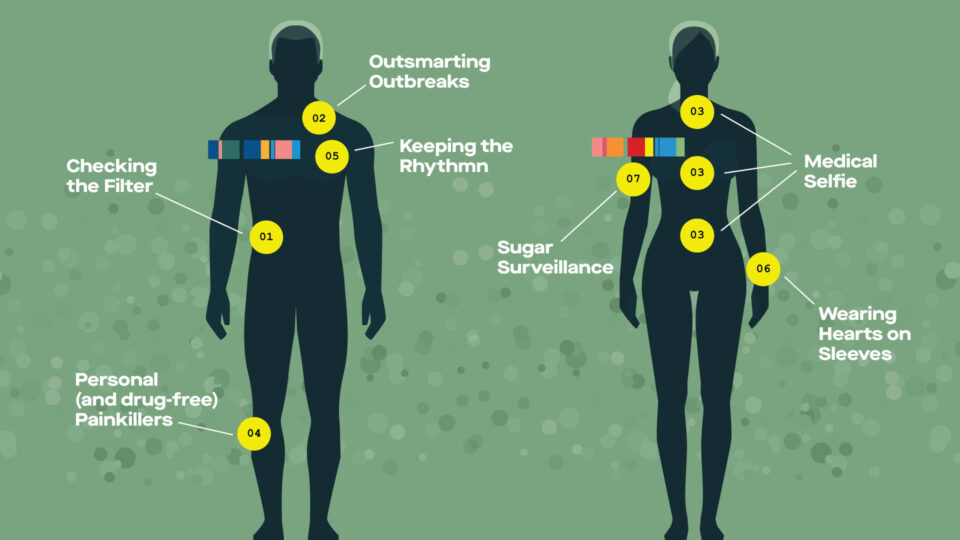
01 – Checking the Filter
Kidney function test kit
An at-home urine test kit that pairs with a mobile phone can rapidly provide a picture of kidney health. This tool, which uses a color-changing strip that’s photographed with a phone and uploaded to an app, can be provided to patients with hypertension or diabetes who are at high risk for kidney disease, a serious condition in which kidneys lose their ability to remove waste from the body and balance fluids.
By detecting elevated levels of proteins in urine, the tool can help identify kidney abnormalities early, when there’s time to intervene before kidney failure occurs.

Approximately 30 million Americans have chronic kidney disease.
90%
Nearly 90 percent of people with chronic kidney disease don’t know they have the condition, as symptoms often emerge after kidneys are significantly impaired.
02 – Outsmarting Outbreaks
Vital sign biosensor
With the ability to remotely monitor an individual’s vital signs—such as respiratory function, heart activity and body temperature—scientists and clinicians can gather key patient data and change treatment plans even from thousands of miles away.
Field-work scientists from Scripps Research are assessing wearable patch technology in Sierra Leone to precisely track disease symptoms in patients with Lassa fever, an acute hemorrhagic fever caused by the Lassa virus. By accessing data from the patch, caregivers can examine patients continuously and intervene if a patient is in distress.
With the help of machine-learning tools that analyze the vast pool of data from these devices, researchers can also identify patterns of infectious disease progression, which can then be used to improve care on a local or global scale.
15-20%
Roughly 15-20 percent of patients hospitalized for Lassa fever will die from the illness, typically within two weeks after symptoms begin.
High risk of infection and tough environmental conditions in outbreak zones present barriers to sustained patient care.
03 – A Medical Selfie
Smartphone ultrasound
A handheld, portable ultrasound device is used with a smartphone to generate high-resolution, clinical-grade images of almost every tissue in the body. This device holds potential to overhaul the way we monitor pregnancy, examine the thyroid gland or even diagnose gallbladder disease.
By enabling fast, on-site biological imaging, this technology provides a mobile solution for a wide range of clinical research projects and can bring medical assessments to more remote communities.
“With every patient I see as a cardiologist I use a smartphone ultrasound for their heart exam…
I haven’t used a stethoscope in 10 years.”
Eric Topol, MD
Scripps Research Translational Institute
04 – Personal (and drug-free) Painkillers
Pain relief cuff
A lightweight cuff uses neurostimulation technology to train the body to produce its own natural analgesic chemicals. Scientists and clinicians at Scripps Research Translational Institute are assessing whether these tools can help young children with sickle cell anemia, cystic fibrosis or cancer manage chronic pain, which can be debilitating at times.
By personalizing pain management approaches with digital technologies, the side effects of traditional opioids can be avoided, and suffering can be prevented for children and their families.

Enduring pain is one of the most feared and challenging symptoms of various chronic diseases.
Novel technologies can revolutionize the treatment of pain and help stop the opioid epidemic.
05 – Keeping the Rhythm
Electrocardiogram (ECG) patch sensor
A small, non-invasive chest patch can be used for patients with atrial fibrillation, an irregular heartbeat that often results in poor blood flow. The sensor essentially acts as a mobile electrocardiogram, or ECG, measuring the electrical activity of the heartbeat.
The Scripps Research Translational Institute uses this technology in clinical trials to monitor heart rhythms continuously across multiple days, allowing them to detect and measure atrial fibrillation episodes that would previously only be captured at a doctor’s office. Earlier detection of the disorder and better identification of subtypes leads to personalized interventions that can dramatically reduce the risk of stroke.

Approximately
1 out of 5
of all strokes are attributed to atrial fibrillation.
23%
Lifetime risk for atrial fibrillation for those with an optimal health profile
38%
Lifetime risk for people with at least one risk factor.
06 – Wearing Hearts on Sleeves
Smartwatch
A digital wristwatch assesses daily physical activity and sleep patterns, and continuously monitors heart rate and blood pressure.
Participants who have enrolled in the All of Us Research Program are able to share their own activity data with researchers in the name of science. The Scripps Research Translational Institute is leading key aspects of this unprecedented, nationwide study that explores the relationship between key biological indicators and other critical health outcomes.
Instead of limited biological snapshots in a clinical setting, comprehensive real-world data provides important insights into how individual differences in genes, environment and lifestyle can influence health and disease.

Detecting early signs of hypertension, or abnormally high blood pressure, can reduce the global burden of cardiovascular disease, which caused more than 17 million deaths worldwide in 2017.
1 in 3
adult Americans have high blood pressure, which can lead to heart disease.
07 – Sugar Surveillance
Continuous glucose monitor (CGM)
Among those with diabetes, blood sugar levels are too high and must be tightly controlled. A biosensor placed under the skin can track blood glucose levels in real time, 24 hours a day. Clinical scientists can use this tool to examine the daily glucose profiles not only of diabetic patients, but also of obese individuals and healthy people, to expand their understanding of how different people respond to foods, exercise and life stressors.
The sensors provide immediate feedback and result in data-rich records that support recommendations for lifestyle changes or other interventions to prevent metabolic disease. Existing treatment strategies can be refined for those with sub-optimal glycemic control.
Without continuous monitoring, dangerous glucose spikes and drops can go undetected.
More than
1 in 3
U.S. adults have pre-diabetes, increasing their risk of type 2 diabetes, heart disease and stroke.